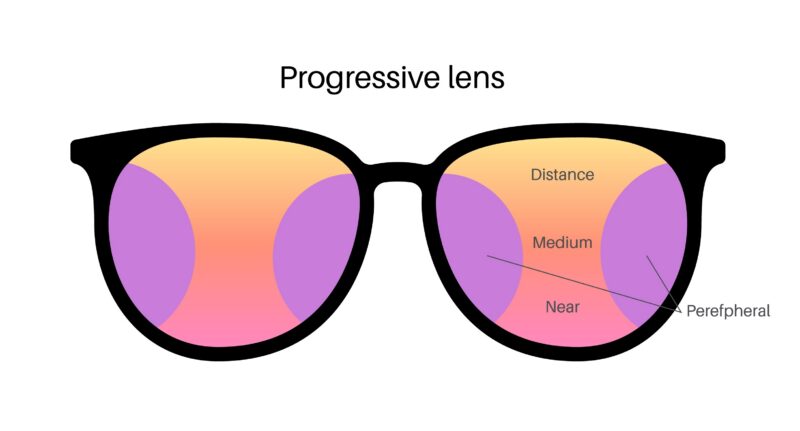
Progressive Lenses Troubleshooting: How to Fix Common Patient Complaints

Progressive lenses don’t usually fail randomly. When patients struggle, there is almost always a clear reason – and in most cases, it can be identified and corrected.
In daily practice, complaints tend to sound similar:
“Something feels off.”
“I can’t find the right spot.”
“These don’t feel like my old lenses.”
These are not vague reactions. They are precise signals. The challenge is not whether a problem exists – it’s whether the practice can interpret it correctly.
This guide breaks down what progressive lens complaints actually mean, where they come from, and how to resolve them without guesswork or unnecessary remakes.
Why Progressive Lens Complaints Are Predictable
Progressive lenses are one of the most sensitive optical systems used in everyday vision correction. They rely on alignment between lens design, frame position, measurements, and patient behavior. When one variable shifts, the system still works – but no longer feels intuitive.
What patients experience is not always blurry. More often, it is effort. Vision becomes something they manage instead of something that happens naturally.
A patient who says “I can see, but it feels uncomfortable” is usually describing increased cognitive load. Their eyes are compensating for a mismatch in design or positioning.
From a clinical perspective, this is useful. Complaints are not noise – they are diagnostic data.
The Most Common Progressive Lens Complaints (And What They Actually Mean)
When patients describe issues, the wording may vary, but the underlying patterns are consistent.
“I can’t find the right spot” usually indicates that the usable zones of the lens are not aligned with the patient’s natural gaze. The corridor may be too narrow, too short, or positioned incorrectly relative to the frame.
“Everything feels distorted when I walk” points toward peripheral distortion becoming noticeable. This is often linked to corridor design, but it becomes significantly worse when fitting height or frame tilt is off.
“Reading is clear, but the computer feels uncomfortable” suggests a mismatch in intermediate zone positioning. The patient is able to access near vision but struggles to stabilize mid-range tasks, which often reflects lifestyle misalignment rather than a defect.
“These feel worse than my old lenses” is rarely about regression in quality alone. It usually reflects a change in design type, corridor length, or lens category that was not properly explained or matched to expectations.
“I feel off balance” is one of the most important signals. It typically points to fitting errors, especially height or frame position, or excessive peripheral distortion that the patient cannot adapt to naturally.
Each of these complaints maps to a specific part of the system. The key is not to generalize – but to interpret precisely.
Root Causes: Where Progressive Lenses Fail in Practice
Most progressive lens issues come from a small number of root causes that tend to overlap.
Measurement inaccuracies are one of the most common triggers. Even small deviations in PD or fitting height shift the usable zones of the lens. The lens is still technically correct – but functionally misaligned.
Frame selection and adjustment play a bigger role than many practices assume. A frame that sits too low, too flat, or too far from the face changes how the patient accesses different zones. The lens design does not change – but its effective performance does.
Lens design itself is another critical factor. Standard designs may not provide enough corridor flexibility for modern visual behavior, especially for patients who spend significant time at intermediate distances.
Material and coating also influence perception. Lower optical clarity or higher reflectance can create subtle instability that patients interpret as discomfort. If you want to understand how material choice contributes to this, it’s worth reviewing how different lens materials affect clarity and adaptation:
https://mialab.com/lens-material-guide-choosing-the-best-lens-material-for-every-prescription
The same applies to coatings. Glare, reflections, and cleaning difficulty all shape how the lens is perceived in daily use:
https://mialab.com/anti-reflective-coating
These factors rarely act alone. They compound. And that’s where small issues become noticeable problems.
How to Diagnose Progressive Lens Problems Step-by-Step
A structured approach removes guesswork and reduces unnecessary remakes.
Start by identifying when the problem occurs. If discomfort appears while walking, the issue is likely peripheral distortion or fitting alignment. If it appears at a computer, the intermediate zone is the priority. If it appears during reading, near zone access needs to be evaluated.
Next, verify measurements and frame position. Check fitting height, PD, pantoscopic tilt, and vertex distance. Many issues can be traced back to small deviations here.
Then evaluate whether the lens design matches the patient’s actual lifestyle. A patient working eight hours at a screen will not succeed with a design optimized for distance-heavy use.
After that, assess whether material or coating could be contributing to instability, glare, or visual fatigue.
Only after these steps should a decision be made between adjustment, redesign, or remake.
How to Fix Progressive Lens Issues Without Immediate Remake
A large percentage of progressive lens complaints can be resolved without replacing the lenses.
Frame adjustments alone can significantly improve performance. Increasing pantoscopic tilt, improving frame stability, or adjusting how the frame sits on the face can realign the corridor with the patient’s natural gaze.
In some cases, re-measuring and slightly adjusting fitting parameters is enough to resolve the issue, especially when the original deviation was small.
Equally important is resetting expectations. Patients who expect “perfect vision everywhere instantly” are more likely to perceive normal adaptation as a problem. Clear explanation often reduces perceived discomfort.
The key is to treat the issue as a system problem, not a product failure.
When a Remake Is the Right Decision
There are situations where adjustments will not solve the issue.
If the lens design does not match the patient’s lifestyle, if the corridor is fundamentally incompatible with their usage patterns, or if expectations cannot be met within the current configuration, a remake becomes the correct decision.
The mistake many practices make is repeating the same configuration with minor tweaks. That rarely changes the outcome.
A more effective approach is to change one core variable intentionally. This may involve switching to a different design category, upgrading to a digital freeform progressive lens, or adjusting material and coating to improve overall perception.
A remake should not be a reset. It should be a correction.
The Role of Digital Freeform and Personalization
Standard progressive designs are built for averages. Patients are not.
Digital freeform technology allows the lens surface to be calculated based on prescription, frame, and usage conditions. This does not eliminate distortion, but it allows it to be managed more effectively.
If you want a deeper technical understanding of how this works, see:
https://mialab.com/what-is-freeform-technology-in-optical-lenses
More importantly, personalization aligns the lens with how the patient actually uses their vision. That alignment reduces adaptation time and improves long-term comfort.
In practice, this is often the difference between lenses patients tolerate and lenses they trust.
How Your Optical Lab Impacts Outcomes
Even the best lens design can fail if execution is inconsistent.
Progressive lenses require high precision in surfacing and finishing. Small deviations affect corridor placement, clarity, and overall stability.
Consistency in manufacturing ensures that lens geometry is repeatable, coatings perform as expected, and turnaround times remain predictable. Without that consistency, variability increases – and variability is one of the main drivers of remakes.
For independent practices, the choice of lab is not just operational. It directly affects patient experience.
If you’re evaluating your current setup, this is a useful reference point:
https://mialab.com/how-to-choose-the-best-optical-lab
A strong lab partner reduces friction behind the scenes – and that becomes visible to patients.
Preventing Complaints Before They Start
The most effective way to handle progressive lens problems is to prevent them.
This begins with setting realistic expectations during the exam. Patients should understand that progressive lenses require adaptation and that initial awareness of different zones is normal.
It continues with aligning lens design to lifestyle early, rather than defaulting to a standard option.
And it depends on clear, confident communication. When patients understand what to expect and why a specific design was chosen, they are far more likely to adapt successfully.
FAQ: Progressive Lens Problems and Solutions
- How long does adaptation take?
Most patients adapt within several days to two weeks. Longer adaptation usually indicates a mismatch in fitting or design. - Do progressive lenses always have distortion?
Yes, in the periphery. The goal is not to eliminate it, but to control where and how it appears. - Can progressive lenses be adjusted instead of replaced?
In many cases, yes. Frame adjustments and measurement corrections solve a significant portion of complaints. - What is the most common cause of failure?
Misalignment between lens design, fitting, and patient behavior – not a single defect.